Click on image above to enlarge
return to: Salivary Ultrasound
see also: Botox injection to salivary glands for hypersalivation
Technique
- Begin with diagnostic ultrasound evaluation
- Needle placement with ultrasound guidance
- May or may not instill lidocaine with epinephrine along the anticipated needle tract with ultrasound guidance (without entering the node/nodule)
- Consider use of color Doppler imaging to identify prominent vasculature in the expected needle path and near the target
- May advance the needle along the long axis of the probe to image the entire shaft
- In general - hold the needle at a 45 dgree angle
- understand the width of the transducer imaging is 1 mm (width of a credit card thickness)
- bevel of the needle pointed toward the transducer to increase echogenicity of needle tip
- Options for fine needle aspiration
- As per Houlton (2015) - Long axis - with combination of capillary action and aspiration
- Capillary: Back and forth action of 22 gauge 1.5 inch long needle to 'shave the cells' along the needle path in the lesion with 'holding the needle in place for a short time'; rotation of the needle within the specimen before removal
- Aspiration: Next two or three passes use suction aspiration with a 3 cc syringe filled with 1 cc of air - with 2cc of negative pressure applied once needle is in nodule with back and forth action; release negative pressure before withdrawl of needle
- As per Ahn et al (2015) Long or short axis with no aspiration (just capillary action)
- Use high-frequency linear 5-12 MHz guidance for a 1.5 inch 25 gauge
- Suction aspiration technique used only to aspirate cystic contents or when scant cellular material expected on first pass
- Long or short axis method used depending on tumor location
- As per Degirmenci et al (2007) study of needle sizes 20, 22, 24 gauge comparing capillary versus aspiration action (thyroid nodules)- resulted in recommendation for thin (24-25 guage) needle and capillary action
- Local anesthesia not applied routinely
- Nodule localized in transverse plane with transducer adjusted to center of ndule in sonographic image (freehand biopsy technique)
- Long axis approach preferred: Needle inserted obliquely along path parallel to the imaging plane (tip and shaft continuously visualized during biopsy)
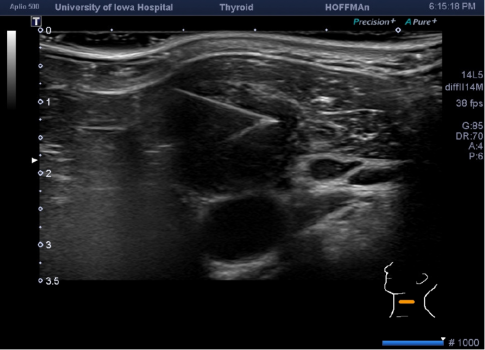
- Short axis approach: needle entrance point in the middle of the transducer surface with the nodule is in the center of the sonographic image - with tracing the needle shaft during advancement and tip seen as a bright echogenic focus
- Used as alternative to long axis technique when
- vessels or the trachea lay in path of needle or
- when transducer had to be tilted to visualize nodules behind bony structures
- Used as alternative to long axis technique when
- As per Houlton (2015) - Long axis - with combination of capillary action and aspiration
- Options for core needle biopsy
- Indications for core needle biopsy: suspected lymphoma, anaplastic carcinoma, and lesions with unsatisfactory results in ultrasound-guided fine needle aspiration biopsy (Gharib et al 2010)
- As per Ahn et al (2015)
- use disposable 18-guage, double-action, spring-activated needle with a 1.1-cm excursion length
- 1% lidocaine mixed with 1:100,000 epinephrine injected at site of needle puncture and around target lesion and along path of biopsy using ultrasound (high-frequency 5-12 MHz transducer
- core needle placed in a parallel fasion under ultrasound guidance advance to margin of or into the tumor
- stylet and cutting cannula of the needle are fired sequentially with core needle usually passed twice
- compression on biopsy site for 20-30 minutes
References
Houlton JJ and Steward DL: Ultrasound Imaging of the Neck Chapter 115 pp 1773 to 1786 in Cummings Otolaryngology–Head and Neck surgery 6th Edition Copyright 2015 Elsevier Saunders Philadelphia
Knappe M, Louw M, Gregor R: Ultrasonography-guided fine-needle aspiration for the assessment of cervical metastases. Arch Otolaryngol Head and Neck Surg 126:1091-1096, 2000
Hodder S, Evans R, Patton D, et al: Ultrasound and fine needle aspiration cytology in the staging of neck lymph nodes in oral squamous cell carcinoma Br J Oral Maxillofac Surg 38:430-436, 2000
Ahn D, Sohn JH, Yeo CK, Jeon JH: Feasibility of surgeon-performed ultrasound-guided core needle biopsy in the thyroid and lymph nodes. Head Neck 2015 Nov 11
Gharib H, Papini E, Paschke R, et al American Association of Clinical Endocrinologists, Associazione Medici Endocrinologi, and European Thyroid Association Medical Guidelines for Clinical Practice for the Diagnosis and Management of Thyroid Nodules: executive summary of recommendations. Endocr Pract 2010;16:468-75
Ahn D, Kim H, Sohn JH, Choi JH, and Na KJ: Surgeon-Performed Ultrasound-guided fine-Needle Aspiration Cytology of Head and Neck Mass Lesions: Sampling Adequacy and Diagnostic Accuracy. Ann Surg Oncol (2015) 22: 1360-1365
Degirmenci B, Haktanir A, Albayrak R, Acar M, Sahin DA, Sahin O, Yucel A, and Caliskan G: Sonographically guided fine-needle biopsy of thyroid nodules: the effects of nodule characteristics, sampling technique, and needle size on the adequacy of cytological material. Clinical Radiology Volume 62, Issue 8, August 2007, pp 798-803