Click on image to enlarge; advance with cursor over border
Return to: Submandibular Gland Resection; Selective Neck Dissection; Deep Lobe Parotid Carcinoma Ex Pleomorphic Adenoma (containing low grade mucoepidermoid carcinoma) Recovery of Lip Weakness
Modified Operative Note
Indications: Recurrent pleomorphic adenoma (two previous resections from tumor arising in left SMG) for extended level 1 and 2a neck dissection
Procedure Details: After informed consent was reviewed, the patient was brought back to the operating room by Anesthesia and placed in a supine position and padded with a time-out performed. He was intubated, and the bed was turned 180 degrees. The previous scar along the anterior left neck was injected with 1:100,000 epinephrine plain. A 15-blade was then used to incise a strip around the previous scar to ensure removal of all tissue previously in the surgical field (resecting skin, scar, platysma and other tissue as a cuff of previously unviolated tissue around the tumor.
A supraplatysmal plane was created under the superior flap with a combination of sharp and blunt dissection. At the posterior portion of the dissection we came the tail of the parotid gland was partially resected employing bipolar cautery for hemostasis. We carried this up until identification of the marginal mandibular nerve was apparent with need to sacrifice it due to tumor involvement.
Dissection was carried out deeply underneath the mandible.The digastric sling was then identified, and dissection carried both anteriorly and posteriorly along the digastric muscle. We identified the lingual nerve as well as the hypoglossal nerve on dissection around the posterior aspect of the specimen. Frozen section was sent from alongside the lingual nerve that returned as negative, as well as frozen sections as listed below. The extended level I neck dissection was completed with removal of the specimen en bloc. Hemostasis was obtained with bipolar cautery.
Level IIA neck dissection was then performed, with positive identification and preservation of the spinal accessory nerve along the anterior border of the sternocleidomastoid. The internal jugular vein was likewise identified and undisturbed during the dissection. This specimen was also handed off for permanent section.
Two fully perforated 10 mm Jackson-Pratt drains were placed, the posterior drain being the deep drain draining the submandibular region, the anterior drain being the more superficial in its drainage area. The patient tolerated the procedure well and was turned back over to Anesthesia in stable condition.additional summary: Resection performed to encompass entire scar - Including resection of skin incision, all visible/palable scar in an envelope ensured by elevation of skin flaps above platysma and (where tumor abutted skin) soft tissue underlying dermis (exposing hair follicles) with resection of small segment of skin (with frozen section negative); marginal mandibular nerve identified with facial nerve stimulator and sacrifices to permit removal of tumor adequately.
Sutures at submand duct and lingual nerve ganglion included with resection with frozen sections all negative:
adjacent submand ganglion
parotid node (perifacial)
adjacent lingual nerve
duct and suture under lingual nerve
skin overlying tumor
Permanent section:
left level I tail of parotid skin suture inferior
left level IIA
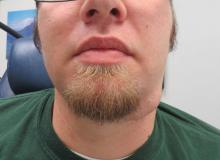
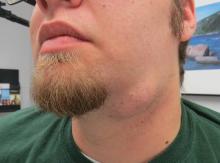
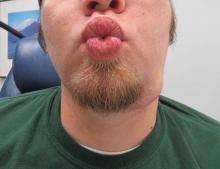
Preop recurrent left submandibular pleomorphic adenoma |
|||
|---|---|---|---|
 |
 |
 |
 |
 |
 |
 |
 |

















