Patient Safety Awareness Week 2019
Anesthesiology and patient safety have been interlinked since at least the 1840s. John Snow, a British physician who is considered one of the fathers of modern epidemiology, also was a pioneer in the use of ether and chloroform as surgical anesthetics. Perhaps most famously, he administered chloroform to Queen Victoria for the births of two of her children. He also traced a cholera outbreak in London in 1854, and his findings inspired significant improvements to water and waste systems in London and around the world. Today, anesthesiology is widely recognized as the pioneering leader in patient safety efforts. It was the first medical specialty to champion patient safety as a specific focus, and the Anesthesia Patient Safety Foundation (APSF) was the first independent multi-disciplinary organization (practitioners, equipment and drug manufacturers, and many related professionals) created expressly to help avoid preventable adverse clinical outcomes, especially those related to human error.
Today: Preventing Complications is Easier than Curing Them
Advances in technology and surgical techniques have resulted in less invasive – and often less costly – procedures. But one anesthesiologist cautions that providers should continue to remain vigilant about potential complications.
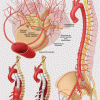
For example, over the past 15 years or so, a procedure called Thoracic Endovascular Aneurysm Repair (TEVAR), in which surgeons access the aorta through a small incision in the groin, has become a popular alternative to open repair, which requires a much larger incision near the site of the aneurysm. The less invasive procedure has definite advantages in terms of shorter hospital stays and recovery times. But the assumption that TEVAR dramatically reduces the risk of spinal cord ischemia has yet to be confirmed.
“There are several management strategies that have to be employed to decrease the risk of this complication,” says Lovkesh Arora, MBBS, MD, clinical assistant professor in the Department of Anesthesia at the University of Iowa who specializes in transplant and vascular anesthesia and critical care medicine.
Arora was lead author of a recent review article summarizing recommendations for properly managing the risks associated with TEVAR in the ASA Monitor, the newsletter of the American Society of Anesthesiologists (ASA), as well as a similar paper in Current Opinion in Anesthesiology.
Although several studies have estimated the overall risk for paralysis or partial paralysis during TEVAR at 10 percent or lower, “that doesn’t matter when it’s you or your family member who was able to walk before the procedure and can’t walk after it,” Arora points out. “The best bet is always to prevent this complication” because paralysis caused by spinal cord ischemia is difficult to treat and recovery time is difficult to predict.
Anesthesiologists can play a vital role in reducing patient risk for spinal cord ischemia and resulting paralysis, Arora says.
“Anesthesiologists need to have a thorough understanding of how inadequate blood flow to the spinal cord can cause damage and of spinal cord protective strategies,” Arora says. Pre-operative planning is key, because it gives the anesthesiologist an opportunity to weigh risks associated with both the patient’s overall health and the extent of the surgery.
“We prefer a team approach,” Arora says. “Discussion between Anesthesia and Vascular Surgery teams prior to the procedure and formulating a plan are vital” to patient safety.
For those patients at high risk of developing some degree of paralysis due to inadequate blood flow to the spinal cord, Arora notes the following recommendations from the ASA, American and the European Society for Vascular Surgery, and other experts in the field:
- Lumbar drain. A lumbar drain is a small, flexible catheter placed in the lower spine to drain cerebrospinal fluid (CSF) that surrounds the spinal cord. Ensuring that CSF pressure around the spinal cord doesn’t become excessive reduces the risk of partial or full paralysis. Arora recommends using a continuous waveform monitor as well, which tells the anesthesiologist whether the drain is actually working properly.
- Blood pressure augmentation. Balancing mean arterial blood pressure with CSF pressure can reduce the risk of inadequate blood flow to the spinal cord during TEVAR.
Other interventions that may be considered for high-risk patients include neurophysiologic monitoring, such as somatosensory evoked potential monitoring or motor evoked potential monitoring, and hypothermia (keeping the patient’s body temperature between the normal 98.6 degrees and about 100 degrees). As a last resort, drugs may be used, but the evidence for them is equivocal, Arora says.
For UI Hospitals & Clinics, Arora and Sundar Krishnan, MBBS, clinical associate professor of anesthesia, have created workshops, online videos and slides for anesthesiologists who don’t do these kinds of cases very often. In addition, the Department of Anesthesia has a pool of faculty who are more experienced in these cases and added a two-week vascular rotation for residents “so that there is a collaborative approach from top to bottom,” Arora says. These efforts also have enjoyed strong support from Mel Sharafuddin, MD, clinical professor and director of endovascular surgery, and others in the Vascular Surgery division and Neurosurgery Department.
“General anesthesiologists are being called more and more frequently for these cases, and we want to make sure everyone knows how to improve the patient’s outcome,” Arora says. “If it’s my family member, I would want these interventions. Even if the evidence for some of the interventions so far is weak, as long as they don’t do any harm, I would rather use these methods to try to reduce the risk.”