return to: Parotid cutaneous fistula sialogram and starch iodine test; Frey's Syndrome Starch Iodine Test Botulinum Toxin Treatment; Salivary Gland Surgery Protocols
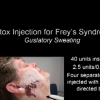
Frey's Syndrome (aka auriculotemporal syndrome or gustatory sweating)
see video for details:
General Considerations
- Frey's syndrome is due to parasympathetic nerve fiber regrowth innervating sweat glands and blood vessels in the facial skin. Produces gustatory sweating, warmth and flushing in the preauricular and temporal area.
- Etiology
- Frequent sequelae of parotidectomy (Watson et al. 2021)
- Other traumatic causes: Incision and drainage of parotid abscess, post submandibular gland removal, mandibular condylar fracture, and obstetric trauma caused by forceps
- Nontraumatic causes: sympathectomy, autonomic neuropathy in diabetes mellitus, herpes zoster infection, and metabolic diseases
- Indications for treatment with intradermal botox injection
- Desire to avoid the sometimes annoying and possibly socially embarrassing dripping of fluid occurring with meals
- Contraindications include:
- Changes to the skin that prevent safe manipulation/injection (infections/inflammation)
- Anatomic changes preventing safe administration to the dermis of the skin (such as proximity of facial nerve in thin damaged skin)
- Potential for acquired resistance due to antibody formation (very unlikely with the doses used)
- Description of technique
- May show video above to the patient and identify it is done in the clinic without general anesthesia unless 'piggy-backed' on to another procedure such as that demonstrated with general anesthesia needed for another purpose.
- Usually do not use general or local anesthesia. For patients in a year or so after parotidectomy, the region to be injected may not have sensation. As sensation returns, it is reasonable to consider application of topical lidocaine (such as topical EMLA cream) if the patient desires
- Describe anticipated effect to last one year (much longer than intramuscular injections) with repeated treatment may be needed
- Per Marchese et al (2023) local treatment through dermal injection with BoNT-A requires multiple injections in a grid pattern due to the short diffusion distance which they report as a 'mean circular area with a radius of 1-1.5 cm"
Preoperative Preparation
- Evaluation
- Identify history of sweating and erythema/flushing of facial skin over parotid bed or neck that occurs during eating
- Minor's starch iodine test.
- The ipsilateral face is painted with iodine and allowed to dry.
- Starch powder is dusted onto the face
- The patient is given a sialogogue (lemon slice, lemon juice, crackers, or any materials that cause the gustatory sweating in an individual patient).
- Dark blue staining reveals the area of gustatory sweating.
- Sequential photographs should be taken at short time intervals and recorded to document areas of sweating.
- Intradermal botox injection
- Ipsilateral face is then cleaned prior to injection.
- Diagram areas of hyperhidrosis based on photos and residual erythema of face
- Alternatively, blotting paper or iodine-sublimated office paper can also be used
- Infrared thermography - initially get temp rise from vascular response, then cooling from sweating. Quantitative.
- Consent
- Describe the procedure - injection of Botox with small needle into the dermis in area of hyperhidrosis localized by the starch-iodine test
- Describe alternative treatments
- Antiperspirants
- Topical anticholinergic medications - do not use in patients with glaucoma
- 1% glycopyrolate lotion
- 3% Scopolamine cream - potential for blurred vision, dry mouth, urinary retention
- Topical aluminum salts - skin irritation
- Explanation of condition and observation
- Surgical treatment of gustatory sweating
- Transcanal neurectomy of the tympanic plexus
- Flap: SMAS flap, Temporoparietal fascia flap, Alloderm interposition
- Risk of facial nerve damage and scarring (Motz and Kim, 2016)
- Temporary effect
- Describe expected sequelae
- Reduction in gustatory sweating for ~ 12 months
- First injection can last much longer (11-27 months)
- Describe potential complications
- Bleeding, infection, reaction to local anesthesia
- Specific: pain related to injection, indiscriminate injection into facial muscles can result in paresis (we have not observed it), acquired resistance to toxin effects
- Unsuccessful or recurrence of Frey's Syndrome
- Can repeat Botulinum toxin injection
Nursing Considerations
- Room Setup
- In Oto clinic room
- Patient positioned upright in chair
- Polaroid camera w/ film no longer available! Hence, digital camera will also suffice
- Materials for starch iodine test: betadine swabs, corn starch, sialogogue (lemon slice or drop)
- Instrumentation and Equipment
- 27 gauge needle, 1 cc syringe, larger needle and syringe to draw up and mix Botox
- Medications
- Botulinium A toxin - dilution used is 2.5 U/0.1ml
- Dose required for denervation is related to target area
- No standard dose that is equally effective for all patients
- Most commonly inject a total of 25 to 40 units per session
- Toxic dose is around 2,500 to 3,000 units for a 70 kg person as per Dhaked et al. (2010)
- Botulinium A toxin - dilution used is 2.5 U/0.1ml
- Prep and Drape
- Remove any residual starch-iodine
- Clearly plan where injections will go
- Drape towels over patient's clothing and leave area of injection exposed
- Use alcohol pad to wipe area prior to injection.
Anesthesia Considerations
- Induction
- Due to small needle and intradermal injection local anesthetic is generally not required
- Positioning
- Patient positioned seated upright in clinic chair with area to be injected fully exposed.
Operative Procedure
- Identification
- Note area to be injected by review of photographs possible marking on face/neck with waterproof maker. Detailed diagram marked out on white board.
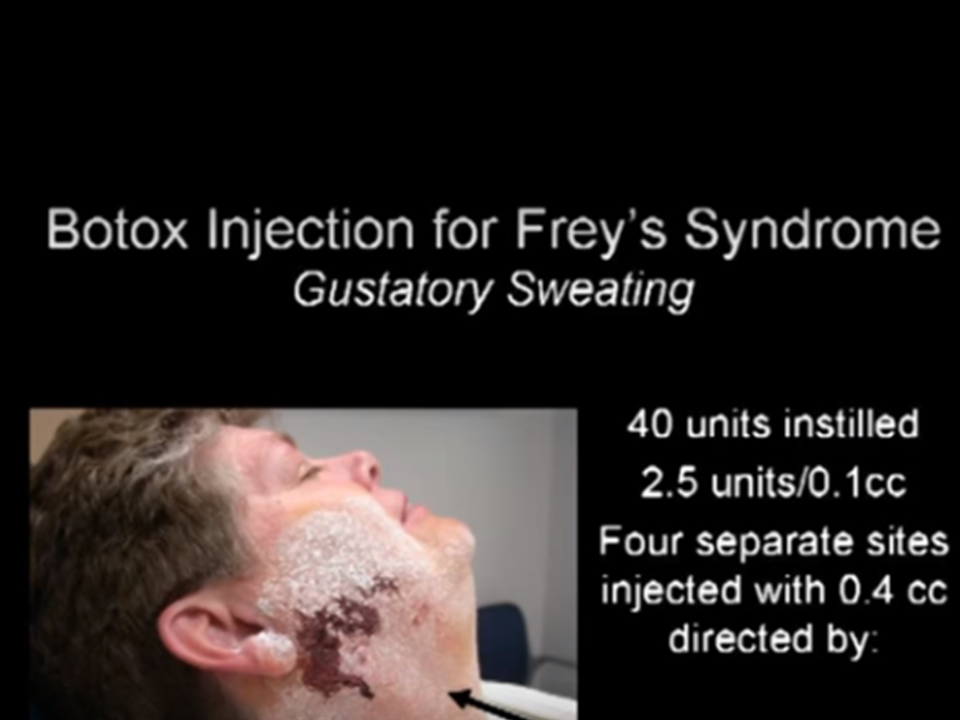
- Injection
- Intradermal injection with 27 gauge needle placed into the dermis up to the hub.
- Botulinum A toxin injected slowly intradermally as the needle is withdrawn.
- Amount to be injected pre-determined, normally 0.2 - 0.4 cc for a total of 5 - 10 units per needle placement (usually 3 to 4 separate needle placements)
- Repeat as necessary in areas of gustatory sweating identified
- Initial treatments after parotidectomy often are painless due to lack of sensation in areas affected. Reinnervation over time may make the needle placement uncomfortable.
Postoperative Care
- Discharge to home after procedure
- Minimal bleeding related to insertion of needle should self-tamponade, wipe with alcohol swab if necessary.
- Follow up as necessary in clinic as outpatient
- One to three days is average time for effects to be seen, most marked at 2 weeks
- Mild pain of injection does not require analgesics
- Followup 3 months after Botox injection (click on image below to start video with audio)
References
De Bree R, van der Waal I, Leemans CR. Management of Frey's Syndrome. Head Neck. 2007 Aug, 29(8):773-8.
Khoo SG, Keogh IJ, Timon C. The use of botulinum toxin in Frey's Sydrome. Ir Med J. 2006 May; 99(5):136-7
Clayman MA, Claymon SM, Seagle MB. A Review of the Surgical and Medical Treatment of Frey Syndrome. Annals of Plastic Surgery. 2006 Nov; 57(5):581-84
Linder TE, Huber A, Schmid S. Frey's syndrome after parotidectomy: A retrospective and prospective analysis. Laryngoscope 1997;107(11):1496.
Steffen A, Rotter N, Konig IR, and Wollenberg B: Botulinum toxin for Frey's syndrome: a closer look at different treatment responses. The Journal of Laryngology and Otology, epub 2011
Capaccio P, Torretta S, Osio M, Minorati D, Ottaviani F, Sambataro G, Nascimbene C, and Pignatraro L: Botulinum toxin therapy: a tempting tool in the management of salivary secretaroy disorders. American Journal of otolaryngology--Head and Neck Medicine and Surgery 29 (2008) 333-338
Cantaraella F, Berlusconi A, Mele V, Cogiamanian F, and Barbieri S: Treatment of Frey's syndrome with botulinum toxin type B. Otolaryngology--Head and Neck Surgery (2010) 143, 214-218
Watson NA, Siddiqui Z, Miller BJ, Karagama Y, Gibbins N. Non-aesthetic uses of botulinum toxin in the head and neck. Eur Arch Otorhinolaryngol. 2021 Nov;278(11):4147-4154. doi: 10.1007/s00405-021-06750-4. Epub 2021 Mar 18. PMID: 33738565.
Motz KM, Kim YJ. Auriculotemporal Syndrome (Frey Syndrome). Otolaryngol Clin North Am. 2016 Apr;49(2):501-9. doi: 10.1016/j.otc.2015.10.010. Epub 2016 Feb 20. PMID: 26902982; PMCID: PMC5457802.
Dhaked RK, Singh MK, Singh P, Gupta P. Botulinum toxin: bioweapon & magic drug. Indian J Med Res. 2010 Nov;132(5):489-503. PMID: 21149997; PMCID: PMC3028942.
Marchese MR, Vollono C, Rigon L, Almadori G, Bentivoglio AR, Petracca M. The Minor's test in Frey syndrome treated with botulinum toxin: Methodology and efficacy. Am J Otolaryngol. 2023 May-Jun;44(3):103818. doi: 10.1016/j.amjoto.2023.103818. Epub 2023 Feb 26. PMID: 36878174.