Return to: Facial Fracture Management Handbook
by Dr. Gerry Funk
Applied Facial Anatomy
Bony Buttresses of the Facial Skeleton
The supporting bony structure of the face can be conceptualized as a system of vertical and horizontal buttresses. The vertical buttresses consist of the paired nasomaxillary (NM), zygomaticomaxillary (ZM) and pterygomaxillary (PM) midfacial buttresses as well as the ramus of the mandible. These buttresses define the vertical height of the face and provide the bony support required for mastication. Masticatory forces imparted to the midface are transferred to the skull base through the ZM, NM and PM buttresses. The ZM buttress often referred to as the key ridge transfers the majority of the masticatory force.

A number of different bones serve to make up these buttresses. The NM buttress is comprised primarily of the maxilla with contributions from the nasal bones and nasal process of the frontal bone. The ZM buttress begins in the region above the first molar and continues up the lateral maxilla through the zygomatic bone along the lateral orbital rim through the frontal process of the zygoma and then through the zygomatic process of the frontal bone. The PM buttress is comprised primarily of the pterygoid plates and to a lesser extent the posterior maxilla. Some of the masticatory forces transmitted to the ZM buttress are dissipated through the zygomatic arch as well as the frontal bone.
The ramus of the mandible imparts some force directly to the skull base through the condylar head and glenoid fossa however it serves primarily to transfer masticatory force to the maxilla. An intact mandibular ramus defines the location of the occlusal plane with reference to the skull base in cases where the midfacial bony architecture has been disrupted. It is in this role that it is primarily conceived of as a vertical buttress of the face (Manson et al. 1980).
The Horizontal facial buttresses are less well known than the vertical buttresses. They serve to impart "cross member" stability to the facial skeleton and define the anteroposterior as well as the horizontal dimensions of the face. The most superior horizontal buttress, the frontal bar, is comprised of the superior orbital rims and the thick frontal bone between them. A second, and the most important horizontal buttress is comprised of the zygomatic arch, zygomatic bone and inferior orbital rim. This buttress is extremely important in defining the anteroposterior position of the malar eminence which is crucial to the restoration of symmetric facial form. The arch of the hard palate and the arch of the mandible (angle, body and symphysis) form horizontal facial buttresses which are important in defining the width of the lower third of the face and occlusal arch.
Orbital Anatomy
The orbit is a conical structure the apex of which points posteriorly. The base is bounded by relatively thick bone contributing to both the vertical and horizontal facial buttresses described above. It is useful to divide the orbit into anterior, middle and posterior thirds (Paskert et al. 1988). The anterior third is comprised of the thick orbital rims and is fractured in association with other named facial fractures such as LeFort II, nasoethmoid, frontal sinus and malar complex fractures. A pure fracture of the orbital rim is an unusual and rare occurrence. The middle third of the orbit is comprised of the thin bone of the lamina papyracea, orbital floor and roof and orbital plate of the greater sphenoid wing. This portion of the orbit is subject to injury in association with the named fractures listed above as well as pure blow out fractures resulting from rapid increases in intraorbital pressure. The majority of blowout fractures affect the floor and medial walls of the orbit. The lateral orbital wall is also subject to medial impaction resulting from forces directed to the lateral orbit. The posterior third of the orbit is made up of the stout bone of the lesser sphenoid wing and body. Fractures of this area require considerable force and frequently are associated with injuries to the orbital contents, including the optic nerve, and intracranial contents.
The posterior orbit serves as the portal of entry from the intracranial cavity for a number of the cranial nerves, most importantly the optic nerve which passes through the optic canal formed in the lesser sphenoid wing. The nerves to the extraocular muscles (cranial nerves III, IV, VI) pass through the superior orbital fissure, which is located between the lesser sphenoid wing and the orbital plate of the greater sphenoid wing.
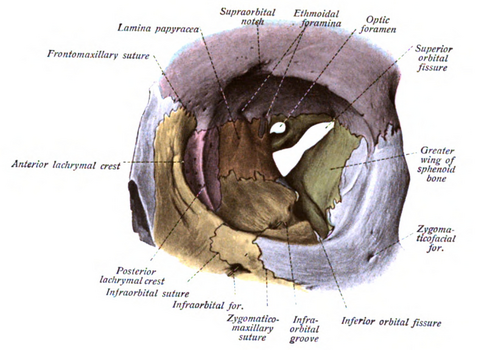
Also traveling in the superior orbital fissure is the supraorbital division of the fifth cranial nerve supplying sensation to the forehead and the lacrimal nerve. The parasympathetic and sympathetic innervation to the eye also passes through the superior orbital fissure. The inferior orbital fissure begins anterior to the foramen rotundum through which the infraorbital nerve (the second division of the fifth cranial nerve) courses.
The optic nerve emerges from the optic canal which is medial and superior in the orbital apex. It takes a lazy "S" pathway to the posterior globe. This redundancy is felt to be important in preventing immediate injury to the nerve if an increase in intraorbital volume causes the eye to be pushed forward. An appreciation of the dimensional anatomy of the orbit is crucial to preventing inadvertent injury to the optic nerve during fracture exploration or reduction. Figure 13 lists some distances worth committing to memory.
The lacrimal canaliculi run from the lacrimal punctae approximately 1 - 2 mm lateral to the medial canthal angle into the lacrimal sac. The lacrimal sac rests in the lacrimal fossa bounded anteriorly and posteriorly by the lacrimal crests. The lacrimal duct which is formed as an inferior extension of the sac runs down through the maxilla to empty into the inferior meatus of the nose. Severe bony trauma in this region may disrupt any or all of these structures.
The canthal tendon serves to suspend the upper and lower tarsal plates across the eye. Clinically, the medial canthal tendon is much more important than the lateral tendon and disruption of the lateral tendon rarely results in significant deformity. The integrity of the medial canthal tendon however is crucial in maintaining a sharp medial canthal angle.
The medial canthal tendon has two slips. The anterior slip inserts onto the nasal and maxillary bones anterior to the lacrimal sac. The posterior fibers insert onto the posterior lacrimal crest. If the medial canthal tendon is disrupted the medial canthal position is shifted laterally and the patient appears telecanthic (has a larger than normal intercanthal distance). This is commonly called traumatic telecanthus if it occurs following facial fractures, most frequently fractures of the nasoethmoid area. Reattachment of the medial canthal tendon to stable bone or secure fixation of small bone fragments to which it has remained attached is important in the aesthetic result following nasoethmoid fracture repair.
Dental and Mandibular Anatomy
The mandible is essentially a rigid arch which is firmly attached to the skull base at both ends. Because the condyles are anchored into the glenoid fossae the mandibular arch and skull base can be thought of as a complete ring and therefore a single fracture line in the mandible is extremely rare and if it does occur usually involves a single condylar process. In general one fracture line results in another fracture line somewhere else in the mandible. For example, mandibular angle fractures are frequently associated with a contralateral condylar neck fractures.
Studies have been performed defining the load bearing force vectors of the mandible in search of the optimal locations for plate placement (Spiessl 1989, Phillips 1992). The main trajectories of masticatory and muscular stresses on the mandible run from the teeth posteroinferiorly and then along the inferior cortex up into the condylar process and to a lesser extent into the coronoid process (Stanley). These studies are interesting, however plate and screw placement is frequently constrained by the location of the inferior alveolar nerve and existing tooth roots. Tooth roots can roughly be assumed to extend into the bone a distance equal to the distance of the mental canal from the top of the mandible. The mental nerve runs along the apex of the tooth roots if dentition is present. Therefore, if screws are always placed below the level of the mental foramen injury to either the nerve or dental structures is unlikely. In selected cases plates placed on the angle of the mandible may be placed superior to the nerve and posterior to dental roots. In the angle region the inferior alveolar nerve enters the mandible approximately in the center of the ramus at the level of the occlusal plane. In the edentulous mandible, alveolar bone loss occurs with time in the absence of dental loading, and the inferior alveolar nerve may come to be very near the upper margin of the mandible and in extreme cases immediately under it.
The fundamental dental anatomy required for this course was reviewed in the introduction section and will not be presented again here.
Frontal Sinus Anatomy
The frontal sinus is an air filled, mucosal lined, variably sized cavity within the frontal bone, the evolutionary function of which is uncertain. The lining of the frontal sinus is cuboidal epithelium; mucus produced in the frontal sinus drains via the nasofrontal ducts into the nose. The term "nasofrontal ducts" is not entirely accurate, because the communication between the frontal sinus and nose is a defined duct in only about 15% of cases. In the majority of cases the communication from the frontal sinus to the nose exists simply as paired openings into the right and left anterior ethmoid labyrinths.
The frontal sinus is defined by three walls: anterior, posterior and inferior. The superior and lateral walls are essentially the narrowed meeting point of the posterior and anterior walls. The anterior and posterior walls are commonly called the anterior and posterior tables. The inferior wall is referred to as the floor. In most cases a bony septum, the intersinus septum, divides the frontal sinus into right and left halves, each side draining independently into the nose. In some cases of trauma only one side of the frontal sinus is affected and can be managed without disruption of the contralateral side.
As was presented in the introduction section, the main concern with frontal sinus fractures is continued drainage of the frontal sinus in order to prevent accumulation of mucus under pressure within the sinus and subsequent formation of a mucocele. If continued drainage of the repaired frontal sinus is in question due to damage to the nasofrontal ducts, all mucus secreting mucosa must be removed and the sinus obliterated. Within the posterior table of the frontal sinus small foramina exist containing veins which communicate with the intracranial dura. These are the foramina of Breschet. Because sinus mucosa may track into these foramina, simply scraping the frontal sinus mucosa from the posterior table at the time of frontal sinus obliteration is not felt to be an adequate means of removing all sinus mucosa. It is advised that the mucosa be scraped from all the sinus walls and then the bone should be drilled smooth with a large cutting and then diamond burr. This is felt to ensure complete removal of all mucosa. The foramina of Breschet may also serve as possible conduits for infection to travel from the sinus into the intracranial space.
References
Manson,P.N., Hoopes,J.E., Su,C.T.: Structural Pillars of the facial skeleton: an approach to the management of LeFort fractures. Plast. Reconst. Surg. 66: 54-61, 1980.
Paskert,J.P., Mansom,P.N., Iliff,N.T.: Nasoethmoidal and orbital fractures. Clin. Plast. Surg. 15: 200-223, 1988.
Spiessl,B.: Internal fixation of the mandible. Springer-Verlag: Berlin, Heideloberg, Germany, 1989.
Phillips,J.H.: Principles of compression osteosynthesis. In Rigid fixation of the craniomaxillofacial skeleton. Yaremchuk,M.J., Gruss,J.S., Manson,P.J. (Eds.), pp 7-14, Butterworth-Heinemann, Stoneham, MA, 1992.
Stanley,R.B.: Pathogenesis and evaluation of mandibular fractures. In Maxillofacial Trauma, Mathog,R.H.(Ed.), pp 136-147.