Return to: Medical Student Instruction
See also: Examination of the subglottis with transnasal laryngoscopy
Introduction to Flexible Fiberoptic Laryngoscopy
Transnasal, without photos - Sobia Khaja MD and Henry Hoffman MD, University of Iowa
- Obtain verbal consent from the patient. If biopsies are to be done in the course of the flexible fiberoptic laryngoscopy, a written consent is required. All consents (verbal and written) generically should including a description of the "Indications, Technique, Alternatives, and Risks". Specifically, the consent for transnasal fiberoptic laryngoscopy should include:
- Indications: Evaluate the voice box, vocal cords and adjacent structures
- Technique: Usually decongest and anesthetize the nose (identify option to defer, to use afrin alone, or a combination lidocaine with phenylephrine. Place scope through nose to perform imaging.
- Alternatives: Indirect mirror exam of the larynx may be possible, but does not permit video-recording and may not permit adequate visualization in all cases. The larynx may better be visualized for some purposes with a rigid videostroboscope (see Videostroboscopy). On occasion (more common in children) imaging of the larynx may require direct laryngoscopy under general anesthesia (see: Microdirect Laryngoscopy). The alternative of not doing it is identified directing the patient to defer if they wish.
- Risks: "Bleeding, infections, reaction to the anesthesia, damage to adjacent structures" including nasal irritation, nose bleed. Reassurance may include comment that our clinic does over 5,000 of these procedure and problems with it are very uncommon - and we can stop the process at any point if you desire. For those patients who have had the procedure done previously, may truncate the consent process, but always ask for permission.
- Usually (not always) spray the nose with lidocaine with phenylephrine, a mixture of a vasoconstrictor and a topical anesthetic, using 0.5 cc on each side of the nose. Always identify to the patient that which you plan to spray in their nose and always get their permission to do so before doing so. Note that the direction of the spray is directed posteriorly -- parallel to the floor and not toward the ceiling. May alternatively use afrin without lidocaine. Note that lidocaine is a vaso-dilator that has been used in microvascular surgery to enlarge blood vessels. As such it tends to congest rather than decongest the nose. A greater degree of nasal opening can often be obtained with spraying with afrin and then later with the lidocaine phenylephrine combination. Usually best to wait several minutes after spraying to permit decongestant and anesthetic to take effect.
- Spray the end of the scope with defogging spray. Other options to defog include the more effective warming of the tip of the scope (may be done under a stream of hot water running from the faucet to the sink). Touching the tip of the scope to the soft palate or base of tongue (usually with the patient requested to swallow) also may work to remove fogging from the tip of the scope.
- Positioning yourself and the patient is important. Stand in front of or to the side of the patient. Instruct the patient to move their hips back in the chair, straighten their back, lean forward and tilt the chin up "as if they are sniffing flowers".
- Advance the scope along the floor of the nose, avoiding the nasal septum. If you are unable to advance along the floor because of a septal deviation or large inferior turbinate you may advance the scope above the inferior turbinate or attempt the contralateral side. The least sensitive part of the nose (and the best to use if possible) is the trough formed by the junction of the maxillar crest and floor of nose (lower, medial aspect of the nasal chamber).
- As the endoscope is advanced to the nasopharynx, instruct the patient to breathe through the nose - most effectively communicated by asking them to 'keep their lips together'.
- Evaluate the nasal chamber and nasopharynx as the scope is being introduced. Advance to the larynx. Inspect the true vocal cords. Inspect for any nodules, polyps, papilloma, leukoplakia, masses, erythema, edema (see: Images of laryngeal abnormalities). When employing the Olympus system in the Otolaryngology clinic, the orientation projected on the screen is similar to a CT scan so that the right vocal cord will be on the left side of the screen and the left vocal cord will be on the right side of the screen (this is opposite from the operating room when doing a direct laryngoscopy).
- As the scope is introduced past the soft palate, instruct the patient to stick out their tongue. This maneuver often (but not always) improves the examination of the base of the tongue and vallecula.
- Instruct the patient to phonate "eee" to allow visualization of vocal cord mobility, making note of incomplete abduction, adduction. The patient can also be instructed to sniff in to allow complete abduction of the cords to allow visualization of the subglottis.
- The best maneuver to evaluate for vocal cord mobility is to have the patient repeated perform the "hee-sniff maneuver". The value of performing and storing a videorecording of the exam (when possible) cannot be over-emphasized.
- Inspect the piriform sinuses. The most effective visualization of the pyriform sinuses comes during phonation with the vocal cords adducted. Other maneuvers may help including having the patient 'blow their cheeks up' to expand the hypopharynx.
- As withdrawing the scope from the larynx, inspect the remainder of the hypopharynx. Examine the nasopharynx including the adenoids and the orifice for the eustachian and nasal chamber as the scope is withdrawn. Example video:
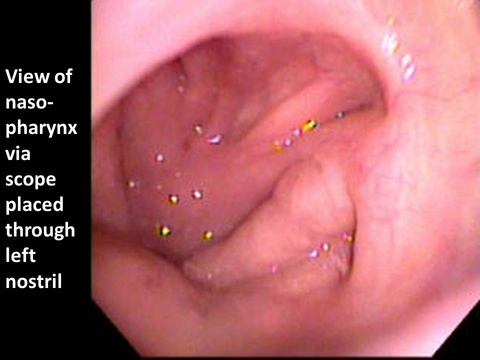
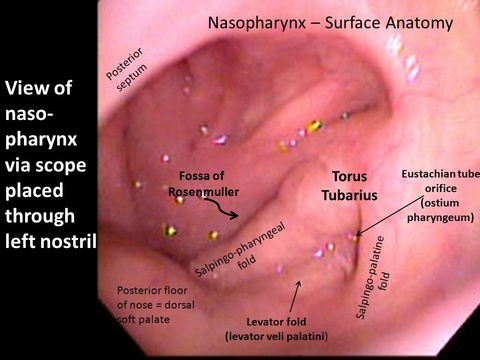
Images
Nasopharynx