See also:
- Nose Bleed Management and Epistaxis Control
- Epistaxis
- Nosebleed - Epistaxis: Sphenopalatine artery ligation (Endoscopic)
General Considerations
- Anterior ethmoidal artery ligation may be considered for continued epistaxis refractory to initial treatments (Seikaly 2021). A strategy that has been employed by some surgeons is to proceed with endoscopic sphenopalatine artery (SPA) ligation for epistaxis refractory to more conservative approaches - external ligation of the anterior ethmoid artery (AEA) and/or posterior ethmoid artery (PEA) may also be considered as well as internal AEA ligation (video pending).
- The anterior ethmoidal artery is an extension of the ophthalmic artery, which is a branch of the internal carotid artery system. As such, this branch is unable to be addressed by embolization techniques. If epistaxis is severe enough to consider addressing the anterior ethmoidal artery, additional consideration of ligating the sphenopalatine artery should be entertained. The posterior ethmoidal artery, also a branch of the ophthalmic artery, is not routinely ligated due to its proximity to the optic nerve and inherent risk of injury to the nerve.
- The anterior ethmoidal artery is identified via subperiostial elevation through a Lynch incision. The artery is approximately 24mm from the anterior lacrimal crest and lies along the frontoethmoidal suture line (Lin 2016). The following drawing demonstrates the artery as a distal branch of the ophthalmic artery
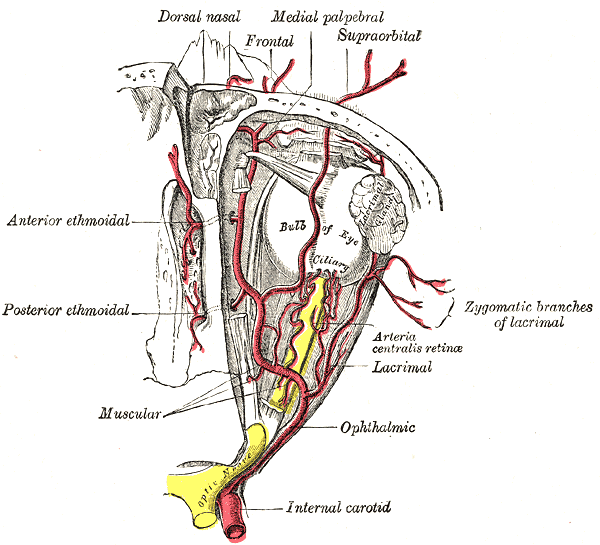
Preoperative Preparation
- Consider CT imaging, if available, to identify the location of the anterior ethmoidal artery pre-operatively (note the distance from anterior lacrimal crest and the height of skull base to help localize intra-operatively)
- If actively hemorrhaging, consider other means of temporizing the hemorrhage while accessing the artery for ligation (i.e. nasal packing or balloon pack).
- Consider pre-op H&H (hemoglobin and hematocrit), type and screen, and transfusion if necessary.
Nursing Considerations
- Room Setup
- Endoscopic sinus surgery setup
- Turn bed 180 degrees
- Arms tucked at patient's side
- Endoscopic sinus surgery setup
- Instrumentation and Equipment
- Endoscopic tower with 0 degree 4mm sinus telescopeStortz endoscopic clip appliers - this is separate from any sinus tray and needs to be ordered specifically "Ethicon Alligator Ligaclip applier"
- Medium clips for clip applier
- Small malleable retractor
- Bipolar cautery
- Medications
- 1% Lidocaine with 1:100,000 epinephrine, off field
- Surgicel, on field
- Bacitracin ophthalmic
- Afrin
Closure
- 4-0 or 5-0 Monocryl / Biosyn for deep closure
- 5-0 fast absorbing gut for superficial closure
Anesthesia Considerations
- Extended tubing for 180-degree turn
- If actively hemorrhaging, rapid sequence intubation may be necessary given potential for swallowed blood and risk of aspiration.
Operative Procedure (Modified)
- A Lynch incision is marked along the lateral nasal dorsum, arcing along the path of the orbicularis oculi. The area is injected with 1% lidocaine with 1:100,000 epinephrine. The area is prepped and draped. A 15 blade is used to incise the skin. The angular artery/vein is often identified just below the skin and should be clipped to prevent bleeding on the field. The incision is carried down to the nasal bone. The incision should remain superior to the lacrimal sac and inferior to the trochlea. A sub-periosteal plane is developed with a cottle between the above anatomical landmarks. The lacrimal crest should be clearly visualized. The frontoethmoidal suture line should then be identified. A small malleable retractor is very useful in retracting the orbit to allow further visualization. At this point, using a 0 degree endoscope will allow for easier visualization of the deeper dissection. Using a cottle or freer, carefully advance down the medial orbital wall along the suture line. The anterior ethmoidal artery is consistently around 24mm from the anterior lacrimal crest or maxillolacrimal suture line. When the artery is identified, a pocket around the artery is created with blunt dissection superiorly and inferiorly. Of note, orbital fat may be seen protruding with the artery as it crosses the periorbita. Endoscopic clip appliers are used to place two clips along the course of the artery between the periorbita and the lamina papyracea. Alternatively, bipolar may be used to cauterize the artery fully. Do not cut the artery, as this increases the risk of retraction and bleeding behind the orbit. The endoscope is removed and the incision is closed with Monocryl/Biosyn and Fast-absorbing gut ensuring that the periosteal layer is closed separately.
- Endoscopic evaluation of the nasal cavity after ligation of the artery is often warranted to ensure epistaxis control.
- Incision along lateral nasal dorsum, carried down to the lacrimal crest. Retraction to expose frontoethmoidal suture line. Anterior ethmoidal artery seen perforating the periorbita and the lamina. Medium clips are placed on the artery in position, without cutting the artery. Incision closed with monocryl deep, 5-0 fast superficially.
Postoperative Care
- Consider removal of nasal packing if adequate epistaxis control is obtained.
- Consider ophthalmology consult vs vision checks
- Bacitracin or erythromycin ophthalmic ointment to incision line
References
Snyderman, CH and Carrau, RL. "Epistaxis." Operative Otolaryngology: Head and Neck Surgery. Eugene N Myers, editor. Saunders Elsevier. 2008.
Lin G, Bleier B. Surgical Management of Severe Epistaxis. Otolaryngol Clin North Am. 2016 Jun;49(3):627-37. doi: 10.1016/j.otc.2016.01.003. PMID: 27267015.
Seikaly H. Epistaxis. N Engl J Med. 2021 Mar 11;384(10):944-951. doi: 10.1056/NEJMcp2019344. PMID: 33704939.
Gray, Henry. Anatomy of the Human Body. 20th edition, 1918. Plate 514. Lea and Febiger, pub. Philidelphia. Public Domain image. Accessed from https:\\commons.wikimedia.org/wiki/File:Gray514.png
Pop SS, Tiple C, Stamate MC, Chirila M. Endoscopic Sphenopalatine Artery Cauterization in the Management of Recurrent Posterior Epistaxis. Medicina (Kaunas). 2023 Jun 12;59(6):1128. doi: 10.3390/medicina59061128. PMID: 37374332; PMCID: PMC10300748.
Rudmik L, Smith TL. Management of intractable spontaneous epistaxis. Am J Rhinol Allergy. 2012 Jan-Feb;26(1):55-60. doi: 10.2500/ajra.2012.26.3696. PMID: 22391084; PMCID: PMC3906521.
Tunkel DE, Anne S, Payne SC, Ishman SL, Rosenfeld RM, Abramson PJ, Alikhaani JD, Benoit MM, Bercovitz RS, Brown MD, Chernobilsky B, Feldstein DA, Hackell JM, Holbrook EH, Holdsworth SM, Lin KW, Lind MM, Poetker DM,
Riley CA, Schneider JS, Seidman MD, Vadlamudi V, Valdez TA, Nnacheta LC, Monjur TM. Clinical Practice Guideline: Nosebleed (Epistaxis) Executive Summary. Otolaryngol Head Neck Surg. 2020 Jan;162(1):8-25. doi: 10.1177/0194599819889955. PMID: 31910122.