(Click on a photo and use the right and left arrow keys to toggle back and forth)
Return to: Laryngeal leukoplakia white plaques on vocal cords or Overview of squamous dysplasia
Go to: Invasive squamous cell carcinoma causing laryngeal leukoplakia
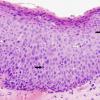
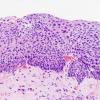
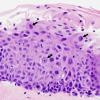
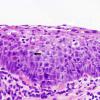
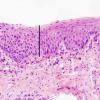
Severe squamous dysplasia and carcinoma in situ are both forms of high grade dysplasia, both carrying significant risk to progress to invasive carcinoma. In fact, both may represent the final observable step before invasion occurs. As such, our convention is to use the terms synonymously, favoring the latter term in the diagnostic line. Our preference is based on the fact that we cannot tell when a high grade lesion is going to invade versus remain confined to the mucosa, especially in its keratinizing form. Most importantly, both lesions should be treated in the same manner by the head and neck surgeon and should be followed closely for evidence of submucosal invasion.
It is important to recognize that this degree of atypia can take various forms and that seemingly lower grades of dysplasia to untrained eyes can be upgraded to carcinoma in situ based on extremes of cytomorphological atypia. On most occasions, the architectural abnormalities easily reach into the upper third of the mucosa and the cytological atypia is severe. Mitoses may be present throughout the depth of the mucosa and abnormal keratinization (dyskeratosis) may be present. Critical examination of the epithelial-stromal interface is imperative to exclude an invasive process.
Conversion from glottis carcinoma in situ to invasive glottis cancer has been reported to occur in 5.4% of 3738 patients identified in the SEER database from 1988 to 2012 (Khaja 2016). When invasive cancer is subsequently found after treatment with a biopsy or excision of CIS it is difficult to distinguish between persistence from incomplete resection versus continued transformation of 'field-cancerized mucosa' (Gailey 2015). Other single institution retrospective cohort studies have described progression to invasive cancer in 11% (Sengupta 2010) and 9.6% (Karatayli-Ozgurosoy 2015). A pooled meta-analysis of 9 studies by Weller et al (2010) reported a 30% malignant transformation of severe dysplasia/CIS. The impact of continued smoking and alcohol consumption is thought to be an important variable increasing the risk of malignant transformation.
References
Khaja SF, Hoffman HT, and Pagedar NA: Treatment and Survival Trends in Glottic Carcinoma in Situ and Satge I Cancer From 1988 to 2012 Annals of Otology, Rhinology & Laryngology 125(4) 2016
Sengupta N, Morris CG, Kirwan J, Amdur RJ, Mendenhall WM. Definitive radiotherapy for carcinoma in situ of the true vocal cords. Am J clin Oncol. 2010;33(1):94-95
Weller MD, Nankivell PC, Mcconkey C, Paleri V, Mehanna HM. The risk and interval to malignancy of patiens with laryngeal dysplasia; a systematic review of case series and meta-analysis. Clin Otolaryngol. 2010;35(5):364-372
Karatayli-Ozgursoy s, Pacheco-Lopez P, Hillel AT, Best SR, Bishop JA, Akst LM. Larygneal dysplasia, demographics, and treatment: a single-instiution, 20-year review. JAMA Otolaryngol Head Neck Surg. 2015;141(4):313-318
“Leukoplakia” (Book Chapter) by Gailey M and Hoffman H in “Sataloff’s Textbook of Otolaryngology” edited by Dr. Robert Sataloff 2015