See also: Thyroglossal Duct Cyst
General Considerations
- Indications
- Infection
- Mass effect (dysphagia, dyspnea, pain)
- Cosmetic
- Contraindications
- Acute infection (treat prior to excision)
- No other functional thyroid tissue (postoperative hypothyroidism). This contraindication is considered only as a relative contraindication. Removal of the thyroglossal duct cyst may still be indicated with the acknowledgement that thyroid hormone replacement may be necessary.
- Medical contraindication to elective surgery
- Embryologic Considerations
- An epithelial proliferation in the floor of the pharyngeal gut appears during the third week of fetal development between the tuberculum impar and the copula. The bilobed diverticulum of primordial thyroid penetrates the underlying mesoderm at the foramen cecum and descends into the anterior neck. The proximity of the pericardium facilitates attachment to either side of the ventral aortic stem so, as the pharynx grows forward, the lobed thyroid primordium descends with the evolving vasculature. The thyroid bud descends with the ventral aortic sac anterior and inferior to the developing second arch. The copula of the third arch, which eventually forms the majority of the hyoid body, is initially posterior and superior to the second arch. Thus, the thyroglossal tract passes ventral to the hyoid bone. The thyroid bud remains connected to its origin during its descent, with formation of a tubular tract.
- The thyroglossal tract path starts at the foramen cecum, runs inferiorly ventral to the hyoid bone and then, at the caudal pole of the hyoid bone, turns initially upward before descending. The thyroid normally takes its position in the anterior neck by the seventh fetal week, with eventual ductile involution. Persistence of the embryonic duct, or portions thereof, may result in thyroglossal duct cysts, or ectopic thyroid, anywhere along the course of glandular descent.
- Other Considerations
- Thyroglossal duct cysts are the most common form of congenital midline neck mass.
- The most commonly found location is just inferior to the hyoid bone.
- The thyrohyoid membrane does not insert on the inferior rim of the hyoid bone. Rather it inserts on the pre-epiglottic tissues and the posterior superior rim of the hyoid. This is important to keep in mind when dissecting the post-hyoid space.
- 30% are discovered by the age of 10; 20% from 10 to 20 yrs, 15% in 30's; and 35% after.
Preoperative Preparation
- Evaluation
- Note cystic mass and movement with deglutition.
- The mass is not mobile in the lateral plane, but moves in the vertical plane.
- Note limits of mass typically within 2 cm of midline.
- Of note, 25% are found just lateral to midline, with the majority of these on the left.
- Examine base of tongue for lingual thyroid (90% ectopic thyroid found at base of tongue).
- Palpate neck for cervical thyroid.
- Consider thyroid scan or ultrasound if normal cervical thyroid tissue not present.
- May use Technetium 99m-labeled pertechnetate scan in children (safer than I 131).
- Alternatively, identify to the patient or family that a hypothyroid state may result from removal of the cyst and is readily corrected with Synthroid.
- Note cystic mass and movement with deglutition.
- Consent
- "Removal of the cyst and tissues that lie along its tract including a portion of the hyoid bone"
- Potential complications
- Bleeding, infection, reaction to anesthesia, scarring
- Damage to adjacent structures: superior laryngeal nerve, hypoglossal nerve (rare)
- Recurrence: 4% for first operations with Sistrunk, higher if portion of hyoid is not removed
- Orocutaneous fistula
- Hypothyroidism
- Need for postoperative intubation or tracheotomy and NG (feeding) tube
- Potential swallowing alteration
Nursing Considerations
- Room Setup
- Instrumentation and Equipment
- Standard
- Special
- Varidyne vacuum suction controller
- Nerve stimulator control unit and instrument
- Bowman lacrimal probes
- Cummings retractor, large and medium
- Bone cutters and rongeurs, small set
- Medications (specific to nursing)
- Antibiotic ointment
- Prep and Drape
- Standard prep, 10% providone iodine
- Drape
- Head drape
- Square off incision site with towels, from lips to clavicles; lateral extension to trapezius
- Split sheet
- Drains and Dressings
- Varidyne vacuum suction or Penrose drain
- Antibiotic ointment to suture line
- Adaptic, small 3 x 3 in
- Fluffs
- Kling, 4 in
Anesthesia Considerations
- General Anesthesia with Endotracheal Intubation
- Positioning
- Modified Rose position with neck extended.
- Using Benzoin solution over chin, affix a 10"x10" drape over the chin.
- Drape to allow easy oral access with minimal drape manipulation.
- Preoperative Systemic Medications
- Antibiotics (see Antibiotic Prophylaxis in Head and Neck Surgery protocol)
- Consider Decadron to reduce postoperative swelling.
Operative Procedure
- Mark incision and infiltrate with 1% lidocaine with 1:100,000 epinephrine.
- Use a horizontal curvilinear incision in skin crease, over mass prominence if no sinus tract/fistula.
- If sinus tract/fistula present, encompass within an elliptical incision.
- Carry incision through platysma.
- Separate strap muscles in midline and retract muscles laterally.
- Incise fascia overlying cyst.
- Retract cyst and free from investing tissues of larynx.
- Incise superior muscular attachments to hyoid without undercutting hyoid or incising periosteum.
- Resect the midportion (10 to 15 mm) of hyoid in continuity with mass using heavy (Mayo) scissors.
- Direct dissection superiorly at 45° angle with respect to long axis of body, with removal of 5 to 10 mm core of base of tongue tissue toward the foramen cecum.
- It is usually not necessary to enter the oropharynx nor remove mucosa. editorial note (HH):
- My practice has been to place a hemoclip to mark the superior extent of the dissection near the foramen cecum.
- I then take a frozen section from the upper end of the resected specimen to search for a patent tract that may occasionally communicate through to the oropharynx.
- If a tract is identified at the superior extent, it is followed as far toward the oropharynx as necessary - and may require entry into the oropharynx.
- If there is entry into the oropharynx, consideration for a feeding tube and even tracheotomy may be entertained.
- Click to see example of infectious complication of incomplete thyroglossal cyst removal with tract communicating into the oropharynx requiring revision surgery.
- Irrigate wound and obtain meticulous hemostasis.
- Place drains, either Penrose or suction drain, depending on size of cyst.
- Close wound in layers.
Thyroglossal Duct Excision
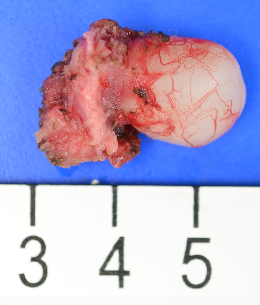
Postoperative Care
- Drains removed when output decreases (typically one to two days).
- Delay oral diet with clear liquids 48 hours postoperatively if pharynx entered.
- Closely follow airway postoperatively.
- Topical wound care
- Follow-up five to seven days for suture removal.
- Check pathology of specimen to ensure benign.
- Follow-up for hypothyroidism (order TFTs if symptomatic).
References
Britnall ES, et al. Thyroglossal duct and cyst. Arch Otolaryngol. 1954;59:282-289.
Hawkins DB, Jacobsen BE, Klatt EC. Cysts of the thyroglossal duct. Laryngoscope. 1982;92:1254-1258.
Hoffman MA, Schuster SR. Thyroglossal duct remnants in infants and children: Reevaluation of histopathology and methods for resection. Ann Otol Rhinol Laryngol. 1988;97:483-486.
Horisawa M, et al. What is the optimal depth for core-out toward the foramen cecum in a thyroglossal duct cyst operation? J Ped Surg. 1992;27:710-713.
Horisawa M, Niinomi N, Ito T. Anatomical reconstruction of the thyroglossal duct. J Ped Surg. 1991;26:766-769.
Katz AD, Hachigian M. Thyroglossal duct cysts. A thirty year experience with emphasis on occurrence in older patients. Am J Surg. 1988;155:741-743.
Lore JM, ed. An Atlas of Head and Neck Surgery. Philadelphia, PA: WB Saunders Co., 1988;674-677.
Meyer CM, Cotton RT. Congenital thyroid cysts and ectopic thyroid. In Falk SA, ed. Thyroid Disease: Endocrinology, Surgery, Nuclear Medicine and Radiotherapy. New York, NY: Raven Press. 1990;381-388.
Pinczower E, et al. Preoperative thyroid scanning in presumed thyroglossal duct cysts. Arch Otolaryngol Head Neck Surg. 1992;118:985-988.
Radkowski D, Arnold J, et al. Thyroglossal duct remnants: Preoperative evaluation and management. Arch Otolaryngol Head Neck Surg. 1991;117:1378-1381.
Sistrunk WE. Technique of removal of cysts and sinuses of the thyroglossal duct. Surg Gynecol Obstet. 1928;46:109-112.
Sistrunk WE. The surgical treatment of cysts of the thyroglossal tract. Ann Surg. 1920;71:121-122.
Hernan Goldsztein, Andleeb Khan, Kevin D. Pereira; Thyroglossal duct cyst excision---The Sistrunk procedure. Operative Techniques in Otolaryngology - Head and Neck Surgery Volume 20, Issue 4 , Pages 256-259, December 2009
