See also: Articles on Music, Hearing Loss, and Hearing Devices
As you read this website, keep in mind the following:
-
People with hearing loss can differ in many ways.
-
Some information may be more applicable.
-
Pick and choose the information most useful for you.
Acknowledgement and Adjustment to Hearing Loss:
The Transtheoretical Model
Successful rehabilitation of adults with hearing loss requires changes in thoughts and behaviors, such as acknowledging a hearing disability, being willing to seek professional help, and completing rehabilitation interventions.
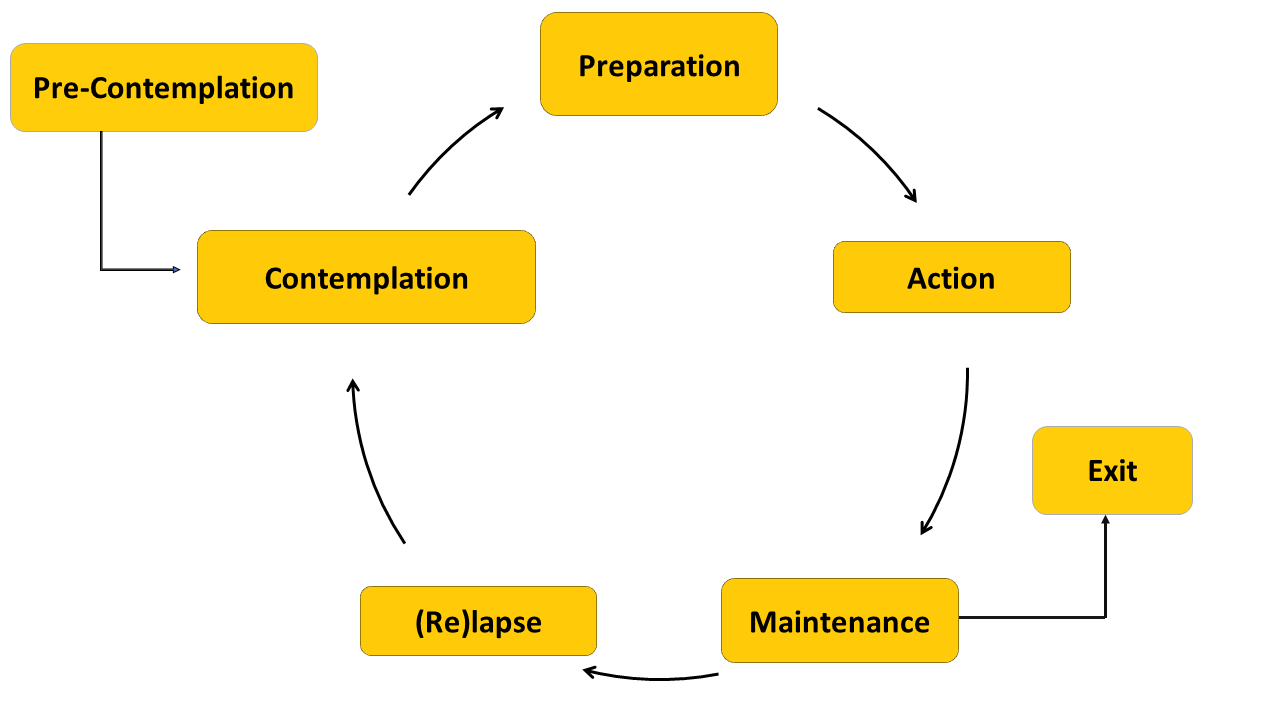
Readiness for making a change is fundamental to persistence and successful aural rehabilitation of music and other auditory input. The transtheoretical model of the stages of change is a method of looking at the changes in attitudes, behaviors, and intentions that are part of readiness for change. This model delineates the cognitive and behavioral processes an individual goes through in making the decision to change a problem behavior related to hearing loss. Like the model of Denial to Acceptance described previously, this model helps clinicians to understand patients' attitudes toward hearing loss, with particular focus on readiness for change and commitment to rehabilitation.
1, 2
This model:
-
helps to explain where patients with hearing loss are at in their hearing healthcare journey and how they respond to rehabilitation recommendations.
-
helps to identify the barriers faced in moving forward.
-
can be used as a framework to develop effective interventions that promote a behavioral change for your clients.
-
helps to identify the steps needed to progress to the next stage.
The Transtheoretical Model
The process through the stages is not necessarily linear. Individuals sometimes cycle back and forth between stages. Each stage represents a time period as well as a set of tasks to be completed in order to move to the next stage. The time spent in each stage can vary from person to person.
-
Precontemplation
Precontemplation is the first stage in changing a behavior.
-
Patients in this stage may:
-
be unaware of or deny a hearing problem, or not ready to make changes.
-
suspect that they have a hearing problem but don't think it is of sufficient magnitude to seek help. – 'My hearing is not that bad,' 'Other people are mumbling, or speaking too softly,' 'I'm too old to change,' 'No one is going to make me change.'
-
believe that they only have difficulty hearing in some situations. – 'I can hear just fine in quiet, but I don't do well when music is too loud.'
-
believe that they do not need to get professional audiological assistance.
-
-
Contemplation
Contemplation involves active consideration of the prospects of change.
-
Patients in this stage may:
-
be ambivalent about making change and wonder 'if things would be any different if I got hearing aids?'
-
look at the personal dimension of the problem as they consider the possibility of changes and its consequence.
-
actively seek out information about hearing health care.
-
begin to evaluate themselves and think more about the pros and cons of the problem behavior.
-
make preliminary moves, such as visiting an audiology clinic for information, participating in a community hearing screening, or talking to friends who wear hearing aids.
-
-
Preparation
In the preparation stage, the individual indicates a readiness to change, which involves attitudes as well as behavior. During this stage, the individual is ready to set goals and priorities.
-
Patients in this stage may:
-
continue to express ambivalence.
-
reach a "tipping point" and decide to act on the hearing loss, but be uncertain of how to proceed.
-
seek professional help or information to support the decision.
-
look for support from the audiologist and others, but also consider the option of "going it alone."
-
-
-
Action
Action involves an overt act of doing something about the problem. During this stage, self-efficacy is crucial. Individuals must believe that they have the ability to make the necessary change. This is a time when support from the audiologist, family, and friends is especially important.
-
Patients in this stage may:
-
be relieved and proud of the decision to act on the hearing problem.
-
worry about not being able to follow through.
-
seek acknowledgment and appreciation.
-
-
-
Maintenance
Maintenance (the last stage) requires using the new behavior for 6 months to 3 years. This change is now part of the individual's life. However, even after 6 months, sustaining a new behavior is difficult, and it is easy to relapse into earlier stages because the problem behavior may not be completely gone.
-
Patients in this stage may:
-
now become a consistent hearing aid user or cochlear implant recipient.
-
be comfortable dealing with their hearing loss, applying self-advocacy strategies, and asking for assistance when necessary.
-
use effective communication/music listening strategies more consistently.
-
feel either successful (leads to "Permanent Exit") or may want to give up (leads to "Relapse")
-
-
-
Relapse
-
Patients in this stage may:
-
not want to wear the hearing device, struggle, and give up.
-
give up attending music programs, or listening to music altogether.
-
feel like a failure and become annoyed and angry.
-
choose to relax and enjoy the freedom.
-
eventually, be motivated to try again.
-
-
Q. How can audiologists assist patients in each stage?
A. Here are some strategies to educate and help move your patients through the stages.
-
Precontemplation stage
-
provide meaningful rationales for change, based on what is important in their life.
-
For example, if they used to enjoy music, what were some particular experiences they currently miss.
-
-
invite family members to attend an appointment to help to facilitate a broader discussion of the patients' potential hearing difficulties in everyday life and how these could be addressed.
-
increase patients' awareness of the negative aspects of the problem and what they are missing out on.
-
-
Contemplation stage
-
listen to the patients and explore their experiences with hearing and communication/music. Below are some prompt questions that you can ask your patients:
-
Ask patients if music listening is important to them. If music is important, ask them about their experience with music and how hearing has impacted them. Below are some prompt questions that you can ask your patients:
-
How has your hearing conditions affected your ability to hear music? Do you have any issues when listening to music?
-
Tell me about your music experience with hearing loss. Has your experience with music changed before and after your hearing loss? How has the hearing loss affected your music experience? (e.g., music listening, singing, playing instruments, etc.)
-
Tell me what your experience has been like when having conversations with music in the background? (e.g., restaurants, parties, weddings, grocery stores, etc.)
-
-
-
provide evidence-based information highlighting the pros and cons of intervention uptake.
-
Provide them with examples from other patients who have been able to improve their communication and music enjoyment.
-
-
Support and acknowledge the patient's increasing awareness of ambivalence.
-
-
Preparation stage
-
provide appropriate educational materials regarding hearing loss, hearing aids, and hearing health care providers.
-
introduce music and hearing loss website to the patients and their families. Click here to access the music and hearing loss website.
-
focus discussion on the benefits of better hearing, and how improving music listening may also improve social life and spoken communication.
-
-
Action stage
-
help the patients to find and enroll in classes on how to use hearing devices and how to live with hearing loss.
-
educate family members about the challenges of hearing loss using hearing devices to support the patients with hearing loss.
-
discuss the importance of self-efficacy in this stage with your patients and refer them to the self-efficacy page of this website. Click here to view the self-efficacy page for patients and their families. Click here to view the self-efficacy page for hearing professionals.
-
-
Maintenance Stage
-
provide follow-up rehabilitation and access to community or online resources.
-
support the patients by discussing strategies in complex listening environments to music.
-
teach self-advocacy strategies to your patients. Click here to view the self-advocacy page for patients and their families. Click here to view the self-advocacy page for hearing professionals.
-
-
Relapse
-
try to refocus on the advantages of better hearing and communication/music listening.
-
try and reduce guilt about the relapse by focusing on prior successes.
-
focus on successful efforts the patient used previously.
-
put a focus on positive experiences, even if they were of short duration.
-
discuss possible new habituation schemes.
-
References
Babeu, L. A., Kricos, P. B., & Lesner, S. A. (2004). Application of the stages-of-change model in audiology. J Acad Rehabil Audiol, 37, 41-56.
Bandura, A. (1994). Self-efficacy. In V. S. Ramachaudran (Ed.), Encyclopedia of human behavior (Vol. 4, pp. 71-81). New York: Academic Press.
Ekberg, K., Grenness, C., & Hickson, L. (2016). Application of the transtheoretical model of behaviour change for identifying older clients’ readiness for hearing rehabilitation during history-taking in audiology appointments. International Journal of Audiology, 55(sup3), S42-S51.
Kaland, M., & Salvatore, K. (2002). The psychology of hearing loss. The ASHA leader, 7(5), 4-15.
Kübler-Ross, E., & Kessler, D. (2005). On grief and grieving: Finding the meaning of grief through the five stages of loss. Simon and Schuster.
Laplante-Lévesque, A., Hickson, L., & Worrall, L. (2013). Stages of change in adults with acquired hearing impairment seeking help for the first time: application of the transtheoretical model in audiologic rehabilitation. Ear and Hearing, 34(4), 447-457.
Mamo, S. K., Reed, N. S., Nieman, C. L., Oh, E. S., & Lin, F. R. (2016). Personal sound amplifiers for adults with hearing loss. The American Journal of Medicine, 129(3), 245-250.
Click here to review references used in preparation of this website.
1. All images on this website are used under Creative Commons or other licenses or have been created by the website developers.
2. Click here to access the sources of images on this page.